WHAT SHOULD YOU KNOW ABOUT SPINAL FRACTURE
Is it back pain or spinal fracture
Physiotherapy helps you…
Spinal compression fractures can be spontaneous. Conditions such as osteoporosis or spinal tumors can weaken the vertebrae in your spine. Once the bone has weakened, it may no longer be able to support your spinal column as you go about your daily activities. In these cases, compression fractures may occur spontaneously when you perform everyday activities, such as:
- Opening a window
- Coughing or sneezing
- Lying in bed
Osteoporotic compression fractures can become recurrent, affecting several vertebrae after the first incident. It is also possible for compressive spinal fractures to occur as a result of high energy trauma, such as from falls or motor vehicle accidents.
See When Back Pain Is a Spine Compression Fracture
Compression fractures are common in the middle and lower back. While a compression fracture can occur anywhere along your spine, the most common areas are in the thoracic and lumbar vertebrae. 60% to 75% of vertebral compression fractures typically occur at the T12 to L2 vertebral levels—your middle back area. 30% of vertebral compression fractures may occur at the L2 to L5 vertebral levels—your lower back area.
These fractures are relatively rare in the neck or upper back. A compression fracture often results in a wedge-shaped vertebral body. This shape is the result of the front of the vertebral bone collapsing (or compressing), while the back of the bone remains unchanged.

Spinal compression fractures may cause localized or radiating pain. Pain and dysfunction from spinal compression fractures typically depend on the number of vertebrae affected and the involvement of any surrounding nervous tissue.
Compression of the vertebra typically causes:
- A dull, deep ache in the region of the fracture.
- Increased pain when the area of the fracture is touched or gently pressed.
- Sudden pains when you take a deep breath, cough, sneezes, and/or move your spine in certain directions.
- If the fracture occurs from a traumatic injury, the skin over the affected vertebra may appear red.
- If the compressed vertebra impinges on a nearby spinal nerve root, one or more of the following additional symptoms and signs may occur:
- A sharp, severe, stabbing pain at the region of the fracture
- Shooting pain that radiates into the arm(s) or leg(s)
- Difficulty in walking
If you have a spinal compression fracture, chances are you are pretty uncomfortable. These fractures are extremely painful, and if left untreated, can severely affect your quality of life.
Can Spinal Compression Fractures heal on their Own..?
Yes, but there are important factors to consider when deciding if you want to get treatment or go it alone. Healing a spinal compression fracture naturally takes a lot of time. On average, spinal compression fractures require three to six months of rest and limited activity to heal completely. Many individuals need a back brace to hold their back in place during the healing process and to protect the site of the fracture.
Waiting for a spinal compression fracture to heal is also very painful, which probably means you’ll need over-the-counter and prescription pain relievers while you heal. Pain is typically in the lower back but can also occur in other areas of the back and even in the neck, hips, thighs and abdomen.
Spinal compression fractures also cause a painful curvature of the spine, causing you to stoop. This forward pitch puts pressure on the nerves that control your legs, which can result in numbness and tingling. Spinal compression fractures also exert pressure on the nerves that control autonomic functions, like bladder and bowel control. This pressure causes urinary and fecal incontinence.
Speed up Healing with Kyphoplasty. Fortunately, people with spinal compression fractures don’t have to wait for them to heal on their own. Kyphoplasty helps to repair the damaged vertebrae and strengthens the area of fracture by using special bone cement and polymers that facilitate bone growth. The Kyphoplasty procedure takes under an hour, and the result is stronger vertebrae and less pain in just a few days.
You’ve got a few key treatment goals when you have a compression fracture of the spine. If you want to ease the pain, heal the fracture, and treat the osteoporosis that weakened your bones and caused them to collapse.
There’s a good chance you won’t need surgery. Most people can get by without it. Compression fractures usually heal on their own in about 3 months. While that happens, your doctor may suggest you try some things at home that can make you feel better, such as pain medicines, rest, physical therapy, or a back brace.
Rest
You don’t want to overdo it with activity, but you also don’t want to stop moving entirely. Lying around for too long can weaken your bones even more. Your doctor might recommend bed rest for a short period of time. After several days or as soon as you start to feel better, gradually ease back into your old routine. For a few weeks or months you may still need to avoid heavy exercise that could make your injury worse. Ask your doctor when it’s safe for you to get active again and what the best ways to get moving are.
Physical Therapy
Once you’re feeling better, ask your doctor if you should join a rehab program or work with a physical therapist.
- Passive range of motion exercise.
- Passive assisted range of motion exercise.
- Active resisted exercise.
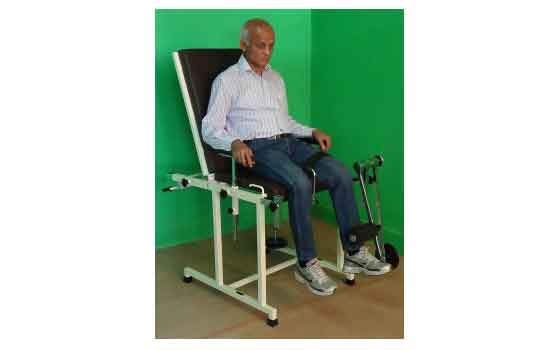
- Exercises that strengthen your back can help you avoid having more compression fractures.
- Balance and proprioception exercise.
- Weight bearing exercise.

- Spinal mobilization exercise.

- Check with your physiotherapy doctor about the best weight-bearing exercises for you, such as:
- Walking
- Yoga
- Dancing
- Strengthening Exercise- There are all good for strengthening bones. Which improve balance and helps in prevent the falls that lead to fractures.
- Bracing- Wearing a back brace when you have a spinal compression fracture is similar to wearing a cast when you have a broken arm. It’s made of a rigid frame that takes pressure off the painful bone and limits your movement. It gives your injured vertebrae — the small bones that make up your spinal column — time to heal.
TREATMENT WITH BESTPHYSIOTHERAPY IN DHKOLI…..
Blossom physiotherapy center is the best physiotherapy center with ultra modular facilities and well experienced staff. Dr. Jyoti Gupta (MPT pediatrics) that is a Pediatrics Physiotherapist as well as a certified Yoga instructor she complete her course from a well known YOGA ALLIANCE INTER NATIONAL FnY STUDIO is a head of the center and senior physiotherapist. She always works on root cause of the disease and treats accordingly. As spinal compression is very serious condition and it needs strict intervention with rehabilitation. Which only provide by experienced physiotherapist. Moreover without rehabilitation an effected person cannot move his/her arms and legs. Unable to stand and even walk. It is only gain by physical rehabilitation but on time if you delay then rehabilitation become difficult. So blossom physiotherapy center provide each and every rehab facilities with ultra modular equipment and technique. In nutshell I will advice must visit the center and have excellence experience. For further information log into blossomphysitherapy.



